Ever since my early days in chiropractic college, I have heard speakers comment on the prevention of surgery with chiropractic care. I have always wondered, however, where the actual evidence was.
In my hospital setting, I routinely evaluate and treat spinal cases with radiculopathy findings that ultimately are seen by a spinal surgeon. So, here is the report of findings for the previous year, July 2006 through July 2007.
We performed a retrospective review and located 162 patients diagnosed with radiculopathy. Data reviewed were initially collected at baseline, during and at the end of active treatment. The treatment basis retrospectively reviewed was manipulation, neuromobilization and exercise stabilization. Of the 162 total cases reviewed, 85.5 percent resolved their radicular complaints. There were three unresolved cases that underwent surgery. This represents 1.85 percent of the 162 total cases, and none of these three cases showed any symptom improvement prior to referral.
 There was one case that was scheduled for cervical spine surgery prior to initial evaluation. The patient elected a trial of 30 days of nonsurgical treatment, which resolved the complaints. This was a 40-year-old female. She had neck pain/headache, intensity 7/10, with left radicular arm pain for approximately six months. She had undergone an epidural injection, which did not help. Our examination revealed left ulnar numbness distribution and left hand weakness. The upper-limb tension A, spurling A, distraction and cervical rotation (less than 60 degrees on the ipsilateral side) were all positive. Wainner1 reports the above cluster of cervical tests has a 90 percent posttest probability that the patient has cervical radiculopathy when all four test positive.
There was one case that was scheduled for cervical spine surgery prior to initial evaluation. The patient elected a trial of 30 days of nonsurgical treatment, which resolved the complaints. This was a 40-year-old female. She had neck pain/headache, intensity 7/10, with left radicular arm pain for approximately six months. She had undergone an epidural injection, which did not help. Our examination revealed left ulnar numbness distribution and left hand weakness. The upper-limb tension A, spurling A, distraction and cervical rotation (less than 60 degrees on the ipsilateral side) were all positive. Wainner1 reports the above cluster of cervical tests has a 90 percent posttest probability that the patient has cervical radiculopathy when all four test positive.
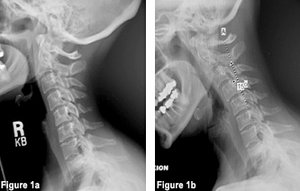
As reported by our radiologist, the radiographs demonstrated straightening of the normal cervical curvature, posterior osteophytes on the left at C4-5, C5-6, C6-7. There was also flexion subluxations note C2 on C3, C3 on C4, C4 on C5 with 15-degree flexion instability at C4-5 during flexion with overpressure (Figures 1a and 1b).
In this case of cervical spine radiculopathy, low-velocity mani-pulation techniques, namely dis-traction manipulation (DM) and motion-palpation technique (MPT), were utilized. The maneuvers were always delivered in a direction that did not cause peripheralization of the pain, which consisted predominantly of cervical lateral flexion and cervical translation.
Neuromobilization was used, which is a manual/exercise-oriented method theorized to mobilize nerve roots that are suspected to be the source of nerve-root pain. It was performed on the ulnar nerve root, which was suspected through examination to exhibit neural tension. With this method, tension was gently applied to the involved nerve roots, which caused mild "pulling," but no pain during in-office treatment. A low-amplitude repetitive movement was introduced in the direction of perceived neural tension for at-home exercise. The complete technique can be performed on any adjusting table, but particularly one with cervical motion that accommodates cervical passive motion during the specific neuromobilization procedure.
The spine stabilization procedures utilized are progressive, meaning beginning procedures are performed prior to intermediate and advanced procedures. The patient was given a handout of each actual procedure, along with a DVD of the procedures to be performed. The patient demonstrated the assigned procedure correctly before they left the office. The cervical spine stabilization progressions utilized were:
- diaphragm breathing;
- spine-sparing strategies;
- cervical centration;
- diaphragm breathing/bracing;
- ulnar neuromobilization;
- active cervical centration;
- wall push-up (scapula stability);
- standing plank;
- neck lift;
- bird-dog extension (beginner); and
- bird-dog extension (intermediate).
What does our evidence show? Other than this one case, it is impossible to determine how many of the resolved cases may have elected for surgery. Recently, Thomas2 assessed the health-related quality of life after lumbar disc protrusion causing radiculopathy (as measured by the North American Spine Society neurogenic symptoms score), treated with either microdiscectomy or nonsurgical care. One-year findings demonstrated similar improvement in both treatment groups and were not meaningfully associated with the treatment received. Perhaps chiropractic needs to step up and offer the nonsurgical solution.
References
- Wainner RS, Fritz JM, Irrgang JJ, et al. Reliability and diagnostic accuracy of the clinical examination and patient self-report measures for cervical radiculopathy. Spine, 2003;28:52-62.
- Thomas KD, Fisher CG, Boyd M, et al. Outcome evaluation of surgical and nonsurgical management of lumbar disc protrusion causing radiculopathy. Spine, 2007;32:1414-22.
Click here for previous articles by Kim Christensen, DC, DACRB, CCSP, CSCS.





