When I went to chiropractic college in the early/mid-1980s, we learned about inflammation in about two pages of Guyton's Physiology. Inflammation was discussed in the context of infection, so there was little context for chiropractors, who overwhelmingly deal with non-infectious musculoskeletal conditions.
Old-World View of Inflammation
With the type of training described above, which is similar today in many respects, the outcome is an inaccurate view of inflammation. The old-world view states that a physical injury occurs (micro- or macro-traumatic), during which cells are damaged and release their contents, which leads to inflammation. The immune system is alerted and arrives on the scene to remove the dead/damaged cells and to clean up the area, which is characterized as the resolution of inflammation and progress toward repair and remodeling.
This view characterizes the dead cells as the ones that cause inflammation because their contents were released during the damaging process. The living cells that arrive are posited to create healing by resolving inflammation and setting the healing process in motion. This basic view is palatable when pain goes away and full function returns.
However, when chronic aches and pains commonly develop, it is often explained that healing has occurred peripherally and now, for some reason, the CNS has become hyperexcitable and is generating pain, even though things are normal in the periphery. This basic view is not palatable at all and represents the old world-view of things inflammatory.
Modern View of Inflammation
It is very common for patients to explain that they individually live with varying degrees of spine and extremity pain. At times the pain is acute, which can compromise activities of daily living, while the pain otherwise is annoying but does not substantially compromise activities or only does so minimally. These same patients often say that NSAIDs provide relief from the acute and chronic pains.
A mistake is to assume that such relief is due to a central analgesic effect because peripheral tissues have not been acutely damaged. The modern view of inflammation demands that we move beyond the superficial notion that cells have to break apart and release their contents as a consequence of injury in order for peripheral inflammation to be present.
In fact, cells that are damaged only serve to briefly initiate an inflammatory process, which is then perpetuated by the "living" cells. In other words, it is the living macrophages, mast cells, fibroblasts, chondrocytes, endothelial cells, platelets, and other cells that drive inflammation by releasing a host of mediators such as cytokines, growth factors, adhesion molecules, free radicals, and dietary fatty acid-derived prostaglandins and other eicosanoids. In the central nervous system, glial cells release similar inflammatory mediators to stimulate the spinothalamic system to generate pain.
Consider your patient population and perhaps even yourself. Is it not true that you and your patients tend to ache more with age? Patients and fellow DCs tell me often that aches and pains are now present in muscles and joints that have not been acutely injured, and that these pains are helped with NSAIDs. It is important to understand that if NSAIDs make one feel better, this means that inflammation is present and being driven by an unhealthy diet.
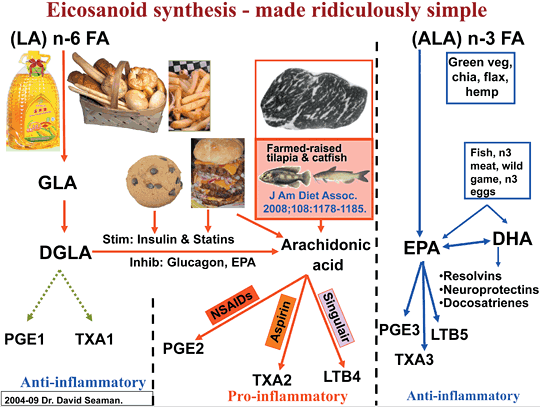
The Diet-Induced Pro-Inflammatory State
In fact, relief achieved by NSAIDs should be considered a dietary sign that demands intervention. This is because NSAIDs inhibit dietary arachidonic acid from being converted into prostaglandin E2, which is released by peripheral cells and glial cells. The figure (above) illustrates the dietary fatty acids that convert into eicosanoids. Arachidonic acid is mostly pro-inflammatory, while dihommo-gamma-linolenic acid (DGLA), eicosapentaenoic acid (EPA), and docosahexaenoic acid (DHA) are anti-inflammatory. These fatty acids become part of the cell membrane phospholipids of the living cells and are released and converted into their respective eicosanoids. Notice the foods that lead to an excessive accumulation of arachidonic acid in our cell membranes.
This type of diet-derived inflammation should be viewed as dietary trauma. We literally "flame up" our cells, so they begin to speak in a pro-inflammatory language that promotes pain and chronic disease expression. And this occurs in the absence of frank injury or damage to cells.
Numerous dietary factors augment the pro-inflammatory state and are present in diets deficient in lean meat, fish, vegetables, and fruit. Without these foods in our diet, we tend to take in excessive omega-6 (n-6) fatty acids, deficient omega-3 (n-3) fatty acids, inadequate potassium and magnesium, inadequate fiber, inadequate bioflavonoids and carotenoids, inadequate vitamins and minerals, and inadequate vitamin D (due to a lack of sunshine mostly). Each of these factors leads to the release of inflammatory mediators in the absence of trauma.
To reduce the diet-induced pro-inflammatory state, we need to do some very simple things. Increase our intake of lean meats, fish, vegetables, and fruit. The best starch source is sweet potatoes. Moderate intake of nuts is also advisable. Avoid or consume only small amounts of sweets and grain products. Support this anti-inflammatory diet with basic supplements such as a multivitamin/mineral, magnesium, omega-3 fish oil, and vitamin D3.
Also on This Topic
- Seaman DR. The diet-induced pro-inflammatory state: a cause of chronic pain and other degenerative diseases. J Manip Physiol Ther, 2002;25:168-179.
- Seaman DR. Nutritional Considerations in the Treatment of Soft Tissue Injuries. In: Hammer WI (editor). Functional Soft-Tissue Examination and Treatment by Manual Methods. Boston: Jones & Bartlett; 2007:717-734.
- Seaman DR. Sports Nutrition: A Biochemical View of Injury Care and Prevention. In: Hyde TE, Gengenbach MS (eds). Conservative Management of Sports Injuries, 2nd Edition. Boston: Jones and Bartlett; 2007:1067-1092.
- Seaman DR. Nutritional Considerations for Pain and Inflammation. In: Liebenson CL.(editor). Rehabilitation of the Spine: A Practitioner's Manual. Baltimore: Williams & Wilkins; 2006:728-740.
Click here for more information about David Seaman, DC, MS, DABCN.





