Empirical clinical evidence, that which is observed over a lifetime of dedicated practice, can be a valuable teacher. Like many other graduating chiropractic students, I had a somewhat simplistic concept of "subluxation," as defined by my instructors.
My first months in practice, however, revealed a very different reality. What I saw most often in my first patients was the exact same pattern of distortion in the spine reappear visit after visit, time after time and with the same levels of intensity. Even though most of my patients did get good symptomatic relief with the work I performed, often becoming completely free of conscious pain, I found myself working continuously on the same patterns of spinal distortions I had identified on their first visit. With symptomatic relief, many failed to return for their appointments. Yet I knew that true rehabilitation and recovery of normal function had been far from complete. As we all realize, temporary symptomatic relief is not true healing. Later, I would hear that a patient's pain had returned, but that he or she had chosen another approach because my work had "helped for a while, but the pain came back." And so I began my quest to further understand this phenomenon called "subluxation." I also came to understand that this was the same condition described as an "osteopathic lesion" by the osteopaths and "facet syndrome" by the medical profession.
I quickly began to realize that I was dealing first and foremost with an inflamed joint structure, and very often it was of a chronic nature. I surmised that the facet malalignment was causing an inflammatory synovial reaction due to the irritation of a buckled joint structure, and that the reaction of the synovial lining of the apophyseal joint was to try and "lubricate" the problem away, as reflected in the normal cycle of synovial fluid production, or simply a reaction to the constant irritation of the injury. With this realization, I then understood that I was dealing with capsular edema, a stretched and swollen capsular ligament structure that I knew to be highly innervated with pain receptors. Thus, I had a good idea where most of the conscious pain stimulus was originating in my patients.
I began to recommend sustained, intermittent cryotherapy via cold pack, 20 minutes on, 20 minutes off, covered, for all of my new patients. Knowing that lowering temperature significantly slows any chemical reaction, I reasoned that cold application would allow the body's natural anti-inflammatory processes to have greater effect. For the most severely disabled, I insisted on complete bed rest and three days' application of this regimen during all waking hours. It was necessary to give these patients two cold packs to be rotated, giving sufficient time for the cold pack to become cold again after use.
The results were remarkable. Not only did my patients avoid the often severely painful reactions to first-time adjustments; they also returned with much less conscious pain and lowered levels of paraspinal and intersegmental myospasm. In severe acute or chronic cases, with lots of guarding myospasm or even a torticollis/tortipelvis, I learned the wisdom of deferring any attempt at adjustment until after a sustained effort at cold pack therapy. My initial treatments consisted of soft-tissue work only. If you have ever been hurt by attempted adjustment in the presence of a severe wryneck or pelvis, you know what I am talking about. Some of us seem to be prompted to "do something" for our fee, even if it defies all logic or further assaults the injured region. Proper patient management in the presence of severe pain and severely inflamed joint structures with guarding myospasm is still, first and foremost, "to do no harm." Many have lost new patients by ignoring this ageless axiom.
In almost all instances, two or three days of bed or recliner rest, immobility, anti-inflammatory agents and repetitive cold pack application would dramatically reduce conscious pain levels and significantly reduce guarding paraspinal or pelvic myospasm. This worked so well over the ensuing years that now, if it is applied properly and does not produce the desired effect, I regard the continuing pain as a red flag, indicative of a disc lesion or pathological process.
As to the phenomenon of guarding myospasm about the spine, we learned in school that this is a primitive reflex, built into the spinal column to protect the spinal cord and nerve roots in case of severe injury or fracture. In my mind, a cervical torticollis or tortipelvis, or even a severely antalgic lumbar spine, must involve such a high level of inflammatory reaction as to illicit the same reflex as a fracture or true subluxation (medical definition). What I also came to realize over time is that this same phenomenon, to a lesser degree, probably accounted for the chronic paraspinal and intersegmental myospasm I always found on palpation above rotated and subluxated facet structures. In almost all instances, this paraspinal myospasm was unilateral and on the side of body rotation. Thus, a right-sided paraspinal and intersegmental hypertonus indicated a clockwise rotary malalignment (cephalic view) and vice versa. On reflection, this only makes physiological sense. The erector spinae function much like guide wires on a tower, and taut wires on one side result in rotary distortion to that side.
With new understanding of the adhesive myofascial change and scarring that develop in and around chronic segmental dysfunction (subluxation), I began to emphasize the importance of rehabilitation exercise to my patients and included prescription for therapeutic paraspinal massage in my regimen of treatments. I also utilized ultrasound, electrical stimulation and intermittent cervical traction. I was looking for reduced levels of recurring paraspinal myospasm, one-sided torque, and facet locking as an indicator of the functional recovery of the spinal segments that had my attention. It seemed logical that the longer a spinal biomechanical lesion (subluxation) existed, the more resistant it would be to correction.
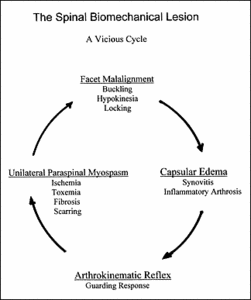
I soon came to realize the truth of this statement and hypothesized that adverse change within the muscle itself, such as toxemia and ischemia, might actually be lowering the threshold of necessary neural stimulus to produce tetanizing myospasm. In other words, as the muscle got "sicker" from its overwork and decreased blood and lymph flow, less reflex neural discharge was necessary to perpetuate the neuromuscular reflex spasm. With this realization, I came to appreciate the cycle of positive feedback loop, which heralds a true pathological process. Only by considering and addressing all the components of this pathological positive feedback loop - facet misalignment, inflammatory arthrosis, capsular edema, arthrokinematic reflex guarding myospasm, unilateral rotary torque and recurring facet misalignment - did I begin to see real objective improvement in the normal tonus of paraspinal tissue and decreased levels of recurring subluxation intensity. I was even able to begin grading these intensities on a scale to chart improvement or regression.
Recognizing the complexity and pathological nature of the spinal biomechanical lesion seems to me to be the first step in addressing all the components that inhibit true rehabilitation and full recovery of spinal segmental function - true healing. To do otherwise is to deny our full duty to our patients.
John R. Bomar, DC
Arkadelphia, Arkansas
Editor's note: A 1978 graduate of Palmer College of Chiropractic, Dr. John Bomar is a past board member of the Arkansas Chiropractic Association and the Arkansas Chiropractic Educational Society. He maintains private practices in Arkadelphia and Hot Springs, Ark.
Dr. John Bomar, a 1978 graduate of Palmer College of Chiropractic, practices in Arkadelphia, Ark. He is a past board member of the Arkansas Chiropractic Association and a founding board member of the Arkansas Chiropractic Educational Society. Contact Dr. Bomar with questions and/or comments regarding this article via e-mail:
.