When the patient appears to have a lumbar disc lesion or injury, how can we help? Many of us use some form of traction. Here is a slightly different take on the possible effects of traction.
I won't go into the technique. I won't try to explain the acronym. I'm more interested in the hypothesis. We all have methods of opening the facets. To quote Mulligan:
"During normal flexion of the spine the disc distorts and becomes wedge shaped. The vertebral bodies proximate ventrally and separate dorsally. The nucleus (or whatever) moves posteriorly, but the disc, whose volume is unalterable, remains under the umbrella of the vertebra above. For this to occur, the facets must be mobile. If the facets are hypomobile, when (lumbar) flexion takes place, the vertebral bodies will be able [to] proximate anteriorly but unable to separate dorsally. The disc may not longer remain under the umbrella of the vertebra above and instead bulge posteriorly, causing symptoms." (See Figures 1-3)
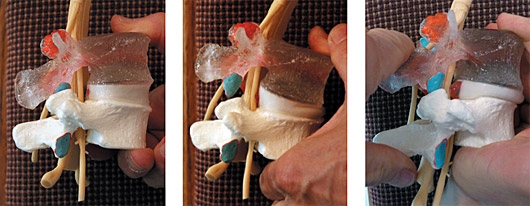
Figure 2: Disc in flexion; note wedging.
Figure 3: Disc in flexion with facets held closed; note bulging and pressure on the anterior disc.
He is saying that when the back side of the disc-facet complex cannot open, abnormal forces are put on the disc. These forces distort the back of the disc in a posterior direction, which is where the nucleus contacts the pain-sensitive annulus; and that this bulge can affect the foramen and the nerve roots.2
Maybe this is why flexion-distraction works so well. Any manual distraction of the spine done from the back is clearly going to affect the facets. The disc itself is fairly deep and harder to directly act upon. Incorporating these concepts, what is the significance of midline tenderness at or between the spinouses? And when the midline tenderness diminishes after traction, does this represent a change in the disc or the facets? Hard to say.
I am not really sure whether this model has been scientifically validated through motion studies. The ideal would be an MRI on patients who have stuck lower lumbar facets, and then a follow-up MRI after manipulation. We might need a motion MRI to be absolutely sure. Does the disc change shape in the patients who get relief?
Over the years, the McKenzie approach has become popular for lumbar discs, especially for self-care. McKenzie emphasizes movement in the direction that reduces the leg pain or centralizes the pain. More often than not, for lumbar discs this is in the direction of extension. The McKenzie term is extension biased. Mulligan acknowledges the utility of McKenzie, but first tests by using motion and pressure to open the involved facets into flexion.
I have been doing various forms of distraction on my disc patients for many years, including flexion-distraction. I will probably continue doing the same techniques, but with a little tweak. I will pay more attention to who responds to flexion or opening of the facets versus those who are much happier going into pure distraction or extension. I've noticed in teaching the modified down dog (wall dog) decompression exercise that some patients prefer neutral spine, and others do better with slight lumbar flexion. Another set of cases in which assess, treat, reassess is the ideal model, as I've discussed in previous articles.
In a similar vein, what about the sacroiliac and its influence on the disc? In the muscle energy model, one of the main lesions on the sacral side of the SI joint is a backward sacral torsion. In this pattern, one side of the sacrum is more prominent and the unilateral lumbosacral joint resists extension (the sacral base cannot nutate forward). This lesion often mimics or accompanies discogenic pain. The therapy is to free the sacral side of the SI and allow it move into extension; another situation in which straight McKenzie extension may not be as effective until you unlock a unilateral joint restriction.
Lumbar Palpation
While we are talking about flexion-distraction, here is another interesting way to use that table. Note: For those of you without flexion-distraction tables, just put a pillow under the patient's abdomen and move their legs to the edge of the table. The idea is to position the patient into flexion and side-bending. You then palpate the lower spine and its myofascial structures on the open side. You've put one side of the posterior muscular structures in a stretch.
As Lucy Whyte Ferguson points out,3 a slight stretch makes the trigger points much more obvious. Pay particular attention to the paraspinal areas and the insertions of the QL into the transverse processes of the upper lumbar spine.
This position is also particularly effective for getting to the origin of the iliolumbar ligament, which starts on the anterior surface of the iliac crest. Robert Kelty, DC, who showed me this particular technique, palpates from the head of the table when he does it, facing the patient's feet. Using your body-weight to push superior to inferior on the iliac crest works well. Changing your typical position and changing the patient's position will definitely change your point of view and what you find.
A Simple Gait Analysis for Frontal Plane Instability
I love this one.4 Is the patient's gluteus medius functioning as they walk? To find out, place 1-inch red dots (or whatever color you choose) on the patient's PSISs. Then watch the patient as they walk away from you. (See Figures 4 and 5) What happens? Opposite the side of the gluteus medius weakness, the red dot will drop inferior if there is dysfunction.
Example: The right gluteus medius is not functioning, allowing a somewhat Trendelenberg gait. As the patient loads onto their right leg in right-stance phase, you'll see the left PSIS (highlighted by the red dots) drop inferior. Ideally, use your video camera to show the patient what is happening.
Gait analysis can be complicated and challenging. This simple look at gait is relatively easy and useful, and it drives therapy. Train the weak side of the gluteus medius. You will help the patient develop increased stability.
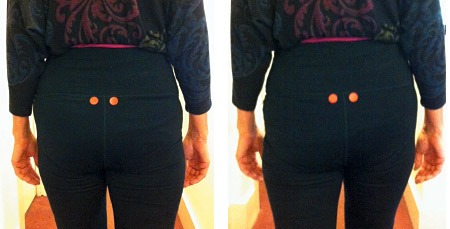
Figure 5: Gait analysis: abnormal response as the right leg goes forward and lands; left PSIS drops inferior, implying functional weakness of the right gluteus medius.
Exercise Rehab for the Back Using Foundation Training
I was just introduced to this concept, developed by Eric Goodman, DC, and Peter Park. It is a fascinating back rehab system; a simple, elegant, effective, yoga-based, weight-bearing functional exercise. Foundation training utilizes body-weight exercises to train the core. The emphasis: powerfully activating the posterior chain.
As always, the key is in the details, which are very well-thought-out in this system. Eric suggests four times more training for the back than for the front. Our lives are spent in flexion. A vast majority of our patients are sitting far too much. When we are upright, we tend to work bent forward. Why not balance this with our exercise routines?
Check out the videos at www.foundationtraining.com. I will do a whole article on this model soon (after I've done the program myself for at least six weeks).
One more thought: Do you have a study group? The first three ideas for this article came from my monthly study group. I meet with other practitioners and share ideas, techniques and cases. We go over mobilization, manual therapy and rehab exercise, and occasionally nutritional gems.
The group includes chiropractors, PTs, MDs, DOs and massage therapists. No room for turf battles; just a mutual sharing. No, I don't teach others high-velocity technique, but there is plenty of material we can share. I appreciate our group as a place I can both share and learn.
Make time to create your own study group. Chiropractors tend to be isolated in our offices; it is great to have a place and time to meet and share clinical material.
References / Endnotes
- Mulligan BR. Manual Therapy: "NAGS," "SNAGS," "MWMs," etc., 5th Edition. OPT, 2004.
- Special thanks to Bill Esser, PT, who introduced this concept to me.
- Ferguson LW. Clinical Mastery in the Treatment of Myofascial Pain. Lippincott Williams & Wilkins, 2004.
- Another gift from Bill Esser, PT.
Click here for more information about Marc Heller, DC.





