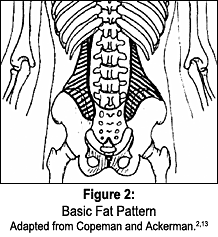
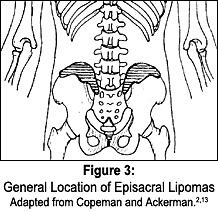
The fat herniation becomes inflamed and swollen under the unyielding capsule and refers pain to the low back, the sacrum, and at times, down into the lower extremities.3 Palpation of the multifidus triangle and PSIS region reveals a firm but moveable nodule, which is generally painful and refers pain on applied pressure. Episacral lipomas are both predictable in location (Figure 3) and tender to palpation, and many other studies show that injection of the lipoma with a local anesthetic takes away the pain for a short time. Excision of the lipoma and repair of the fascial tear may produce a more permanent cure.4
Other terms for the episacral lipoma are the back mouse,5 iliac crest pain syndrome6 and multifidus triangle syndrome,7 but perhaps the best description is lumbar fascial fat herniation.3 The episacral lipoma occurs approximately three times more frequently in women, particularly in moderately obese women.8 Typically, patients presenting with a episacral lipoma have run the gamut of treatment protocols. They may have seen many specialists and been subjected to many examinations and diagnostic tests, all usually with negative results. At times, the only objective findings are decreased motion due to pain, tenderness to palpation and the presence of a nodule at the sacral region. Many patients have had epidural injections without success and the local infiltration with anesthetic is only temporary and expensive.
A client presenting with excruciating low back pain, the presence of an episacral lipoma and reproduction of the pain upon digital palpation alone should lead the practitioner toward the diagnosis of a lumbar fascial fat herniation.
Case Study
The patient, a 50-year-old, right-handed female, presented to my office four months post-motor-vehicle accident. She had been rear-ended and pushed into the vehicle in front of her. Her vehicle was totaled. She experienced immediate neck and low back pain. The patient was being treated at another facility for the intervening period, which included medication, chiropractic manipulation and physiotherapy, and had not been making significant improvement with regard to her low back pain.
She presented with complaints of right-sided low back pain radiating down the right lower extremity to the foot. Radiographs revealed no abnormalities. An MRI revealed the presence of a focal 7-8 mm L5-S1 left paracentral and broad-based central disc herniation pressing upon the exiting left S1 nerve root. This had also resulted in left neural foraminal stenosis and broad-based canal stenosis. The patient had been offered a surgical option that she refused, citing her right-sided pain and that the surgeon offered no opinion as to why her pain was opposite the side of disc herniation. As the patient refused the surgical option, she was then released as having reached "maximum medical improvement."
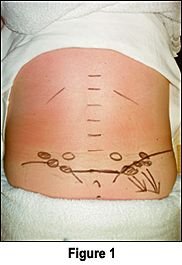
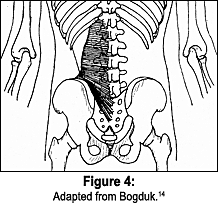
The patient presented to my clinic noting a 10 percent improvement of her low back pain following the prior four months of treatment. Examination revealed lumbar range of motion to be within normal limits, with pain noted upon flexion and extension. Sciatic nerve tests were negative, with primarily low back pain produced. Palpatory examination revealed the presence of multiple large, prominent fat herniations overlying the right iliac crest (Figure 4). Firm pressure on the right-sided lipomas reproduced the patient's complaint of low back pain, right hip and right lower extremity referred pain. Upon deep pressure, the patient exclaimed, "That is exactly where the pain has been since the accident!" It was noted that there were smaller lipomas overlying the left iliac crest; however, these were not tender.
The patient was treated with a combination of chiropractic manipulation, ryodoraku stimulation and trigger point therapy. Electrical stimulation was performed in a "surrounding" distribution, with the lipoma in the center of a circle of points. Considering the patient's MRI results, no rotary lumbar manipulation was performed, however, the patient was manipulated in an anterior to posterior direction. Upon the patient's return visit, she noted a 30% improvement and upon the third visit, noted a 60% improvement in her overall pain condition. After a four-week continuous course of treatment, the patient noted an overall 90% improvement with regard to her initial complaints and was released from care.
In a previous article written for this publication,9 I noted research that suggested a fat herniation could account for a significant amount of low back pain not attributed to a disc herniation. The patient in that case study had previously undergone lumbar discectomy, yet continued to experience significant pain around the episacral lipoma. A local infiltration of anesthetic greatly improved the patient's condition, but did not permanently eliminate the pain. Although the research pointed to torn fascia and herniated, inflamed, fatty tissue as the primary cause of the pain in an episacral lipoma, an orthopedist responded to that article and purported his theory that the pain actually was a result of a disruption of the bioelectric flow between the fascia and the skin, and that the pain occurs when "energy" arcs into the surrounding tissues.10
At first, I dismissed this idea, believing that while it might explain why there is pain in a specific lipoma, it does not explain why the majority of episacral lipomas, as well as benign subcutaneous lipomas, are not painful. As Singewald revealed in his 1966 study, the lipoma is present in 16 percent of individuals, of which only 10 percent elicit pain.8 Curtis suggests that the pain is due to intranodular pressure within the lipoma and its referred pain pattern, in that multiple needle punctures alleviate the pain.11 Over the years, I have tried various manipulations as well as physical therapy modalities in an effort to come up with an accepted working chiropractic protocol. Recently, I've used microstimulation with great success.
Dr. Yoshio Nakatani presented his theory of ryodoraku acupuncture in 1951. He measured the electrical activity of acupuncture points and was first to use electrical stimulation on acupuncture points. Ryodoraku stimulation uses a constant 12V and a current of 200 microamps for treatment. Dr Nakatani found that there are a number of electrically conductive points not associated with any specific acupuncture points, which he called reactive electro permeable points. These points often corresponded to trigger points, and stimulating them with 200 microamps for 7-10 seconds was found to be a very effective form of regional acupuncture.12 This system was renamed "electromeridian imaging" (EMI) by Dr. John Amaro in 1982 and brought to chiropractors through his many acupuncture seminars.
After my own experiments, I believe that the area surrounding the lipoma corresponds to the reactive electroper-meable points. Although it is inconclusive as to whether the microcurrent stimulation or the chiropractic manipulation brought about the most relief to this patient, ryodoraku stimulation can be used on patients who cannot withstand side posture manipulation, as well as those with acute trauma. There are less invasive treatments than local infiltration of an anesthetic which is short-acting and expensive. There are avenues other than the surgical excision, removal of the lipoma and repair of the fascial tear. There are avenues other than disc surgery for pain that is emanating from an episacral lipoma, rather than pain that is entirely discogenic. The episacral lipoma or the back mouse is one condition that can be can be effectively treated using a combination of microcurrent stimulation and spinal manipulation. Since 1937, many studies have been performed by medical researchers on hundreds of patients. Research within the chiropractic community dealing with this important yet overlooked problem is greatly lacking, and is warranted.
References
- Ries E. Episacroiliac lipoma. Amer J Obstet Gynec 1937;34:490.
- Copeman WSC, Ackerman WL. "Fibrositis" of the back. Quart J Med April-July 1944;13:37-51.
- Hucherson D, Gandy J. Herniations of fascial fat. Am J of Surgery November 1948;76:605-609.
- Herz R. Herniation of fascial fat as a cause of low back pain. JAMA 1945; 128:921-925.
- Curtis P. In search of the back mouse. J of Family Practice 1993;36(6):657-659.
- Fairbanks J.O'Brien J. The iliac crest syndrome. Spine 1983;8(2):220-224.
- Bauwens P, Coyer A. The "multifidus triangle" syndrome as a cause of low back pain. British Medical Journal, Nov. 26, 1955:1306-1307.
- Sinqewald M. Sacroiliac lipomata - an often-unrecognized cause of low back pain. Bull Hopkins Hosp 1966;118:492-498.
- Bond, D. Low back pain and episacral lipomas. Dynamic Chiropractic, September 2000;18(19):48-49.
- Nowacek C. Letter to the editor, Dynamic Chiropractic, Dec. 14, 2000.
- Curtis P, Gibbons G, Price J. Fibro-fatty nodules and low back pain. J of Family Practice, April 2000;49(4):345-348.
- Nakatani Y, Yamashita K. Ryodoraku Acupuncture. Osaka, Japan: Royodoraku Research Institute, July 1977:1-6.
- Copeman WSC, Ackerman WL. Edema or herniations of fat lobules as a cause of lumbar and gluteal "fibrositis." Arch Int Med 1947;79:22.
- Bogduk N. Lumbar dorsal ramus syndrome. Chapter 38 in Modern Manual Therapy of the Vertebral Column; Grieve GP (editor). Churchill Livingston, New York, N.Y., 1986.
David Bond, DC
Encino, California